From Flash to IUSS
IUSS grew out of an earlier era of “flash” sterilization, when the priority was keeping procedures moving in urgent situations. It was designed for the unexpected, a dropped instrument, a last-minute need, a case already in motion, not as a routine answer to workflow gaps. But over time, tighter OR schedules, limited inventory, and rising procedural demands pushed many facilities to rely on it more often than intended. The risk to patient safety was clear: eliminating dry time could leave devices wet, creating infection prevention concerns when those wet items were exposed to the environment and presented for use.
As sterile processing practices evolved, so did the understanding that IUSS should remain a true exception, not a daily operating strategy. Moisture is where confidence starts to break down.


When Moisture Enters the Process, Confidence Starts to Leave
Moisture can compromise the sterile barrier and serve as a breeding ground for microorganisms, undermining confidence in the process outcome. Some container manufacturers have suggested that wet outcomes are acceptable because the moisture is “sterile water” generated during sterilization, but that claim ignores an important factor: the effectiveness of sterilization is influenced by how well instruments were cleaned and decontaminated beforehand. Once a container is opened, wet contents are exposed to the environment, making contamination during handling and presentation a significant infection prevention concern. In sterile processing, a dry outcome is not a preference, it is one of the clearest signs that the process has worked as intended and that instruments are ready for safe storage, transport, and use.
Terminal Sterilization Changes the Standard
The goal is not simply to get instruments back to the OR faster. The goal is to return them in a way that supports safety, consistency, and readiness for use. That is why terminal sterilization remains the stronger standard for departments focused on reducing risk and improving workflow reliability. As customers asked for ways to accelerate sterilization and turn over instrument sets with little or no dry time, Case Medical took a different approach. Instead of trying to justify wet outcomes, we validated our SteriTite container system to determine how quickly it could achieve a dry result in steam sterilization while still supporting a terminal, safe outcome. That is what is driving the shift away from IUSS. SPD leaders, technicians, and IP teams need a process that supports speed without sacrificing consistency, sterility maintenance, or control.
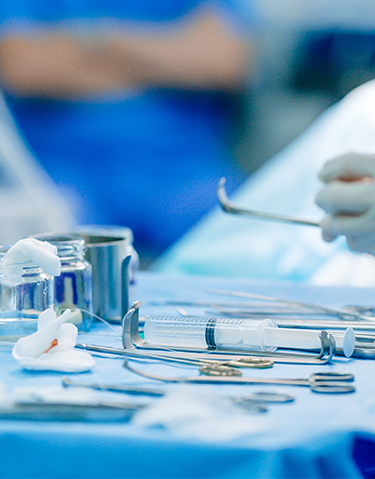

SteriTite Makes the Shift Practical
Case Medical’s SteriTite universal sterilization container system helps make that shift possible with validated 5–8 minute dry times that support terminal sterilization and dry, ready-to-use outcomes. By reducing the risks associated with wet sets and helping departments achieve a safer result faster, SteriTite gives teams greater confidence in storage, handling, and presentation for use. Compatible with all sterilization modalities and cleared for all medical devices, SteriTite also supports standardization while helping sets move through SPD more efficiently. With 2D barcode scanning for digital visualization, SteriTite also adds greater visibility and traceability across the sterilization process, making it a container system designed to improve efficiency while supporting a safer outcome.
The Better Next Step Starts Here
Moving away from IUSS is not just a processing change. It is a shift toward stronger workflow, greater consistency, and better control across SPD. With SteriTite, Case Medical gives departments a way to support terminal sterilization while improving efficiency, reducing waste, and promoting dry, ready-to-use sets.
To discuss how SteriTite can help your team transition from IUSS to terminal sterilization, connect with a Case Medical specialist.